The Big Day
Read about specific aspects of the day of surgery below. Read selected text from Paul Roud’s guidebook (pp. 17-20)
The Consent Form and Letting Go
 When you arrive at the medical facility for ACL surgery, you will register and be asked to sign a consent form. The consent form is intended to inform you of the risks involved. However, it is a legal document and not a helpful way to gather information about the procedure. It is similar to boarding a plane for the first time and having the flight attendant announce before take-off everything that could possibly go wrong with the plane.
When you arrive at the medical facility for ACL surgery, you will register and be asked to sign a consent form. The consent form is intended to inform you of the risks involved. However, it is a legal document and not a helpful way to gather information about the procedure. It is similar to boarding a plane for the first time and having the flight attendant announce before take-off everything that could possibly go wrong with the plane.
The information in the consent form will not tell you what to expect. If you are someone prone to worrying about the worst case scenario, arrange with your doctor’s office to sign the forms well in advance of the surgery. Ideally, you will head into the operation with the expectation that good things are going to happen.
In general, the surgery is very safe, and the chances of anything catastrophic happening are extremely slight. From time to time, however, unpleasant complications do arise. For example, there is a slight risk of infection or nerve or blood vessel injury. Side-effects from the anesthesia, such as a bad headache, are possible. Of course, there are unpredictable risks with this or any surgery.
 Keep in mind that, on average, more than 90 patients out of 100 are satisfied with the operation. At the same time, not every surgery can be picture perfect. The most frequent concern with ACL surgery is some residual loss of motion. While this is rarely a significant problem, it may result in lack of full extension of your leg. About five to seven percent of the time, the new ligament can stretch out more than desired. This means that the stability will be less than ideal. While unlikely, the new ligament may even stretch to the point where it provides little or no support. The normal outcome for most patients, however, is that the reconstructed ligament is stronger and tighter than the original ligament.
Keep in mind that, on average, more than 90 patients out of 100 are satisfied with the operation. At the same time, not every surgery can be picture perfect. The most frequent concern with ACL surgery is some residual loss of motion. While this is rarely a significant problem, it may result in lack of full extension of your leg. About five to seven percent of the time, the new ligament can stretch out more than desired. This means that the stability will be less than ideal. While unlikely, the new ligament may even stretch to the point where it provides little or no support. The normal outcome for most patients, however, is that the reconstructed ligament is stronger and tighter than the original ligament.
Knowing about potential complications can keep you from panicking should they occur. At the same time, you will only create needless anxiety if you focus on them.
Collecting information about ACL surgery is a critical step in the decision-making process. But once the decision has been made and you are heading into surgery, it is time to let go and trust that you have made the right decision. Your doctor and the rest of the medical team want the best for you. Your success is also their success. They will do everything they can to make your experience a positive one.
Which Anesthesia?
You will meet with the anesthesiologist (a medical doctor) before surgery or on the day of surgery. A nurse anesthetist may also participate in your case. The choice of anesthesia (anesthesia means loss of sensation, especially the sensation of pain) is a joint decision among the patient, surgeon, and anesthesiologist. The anesthesiologist, however, may have a clear recommendation based on your health status, the surgeon’s preferences for particular operating conditions, and the drugs available.
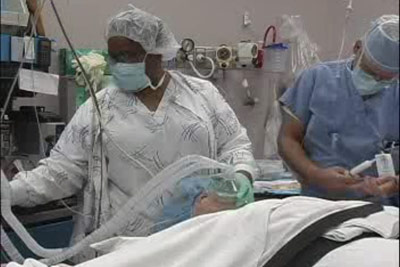
The basic anesthesia decision with ACL surgery is whether to have a general or a regional anesthetic. With general anesthesia, one remains unconscious throughout the surgery and there is no recollection of the surgery afterwards. Before beginning general anesthesia, a sedative is often delivered through the IV (intravenous line). This may make the person sleepy or actually bring on sleep. A face mask may then be put over the individual’s mouth and nose area. In adults, oxygen is delivered through the mask and anesthesia is introduced through the IV. Once the anesthesia has begun, gas may be delivered through the mask or a breathing tube. Individuals respond very quickly to gas—they lose consciousness almost at the onset and regain consciousness very soon after the gas is removed.
The Surgical Procedure
 After registering, you will be asked to go to an area that prepares you for the surgery. Generally, family or friends can stay with you here. You will change into a hospital gown, and your clothes will be stored for safekeeping. Patients are sometimes allowed to wear shorts under their gown if there are no metal closures. This is at the discretion of the medical team. If wearing shorts is a preference you would like to consider, ask ahead of time if doing so is acceptable. A member of the medical team may record your pulse, temperature, respiration, and blood pressure.
After registering, you will be asked to go to an area that prepares you for the surgery. Generally, family or friends can stay with you here. You will change into a hospital gown, and your clothes will be stored for safekeeping. Patients are sometimes allowed to wear shorts under their gown if there are no metal closures. This is at the discretion of the medical team. If wearing shorts is a preference you would like to consider, ask ahead of time if doing so is acceptable. A member of the medical team may record your pulse, temperature, respiration, and blood pressure.
With regional anesthesia, the anesthetic is injected into the spinal fluid (known as a “spinal”) or in the space next to the spinal fluid (known as an “epidural”). The person is essentially numb from the waist down as pain impulses never reach the brain.
For practical purposes, the primary difference between an epidural and a spinal is that a spinal acts more quickly than an epidural. In addition, an epidural can be redosed during the procedure whereas a spinal cannot be. Any discomfort in receiving either a spinal or an epidural should be quite minimal: the skin is numbed before the injection, and often, the person will already have received a sedative.
There is the option of remaining fully awake with a regional anesthetic. However, the prospect of being fully awake and aware of all the activity in the operating room—in particular the mechanics necessary to reconstruct the knee—is outside the comfort zone of most patients. Generally, unless you specifically request to be fully awake, you will receive medication that should leave you feeling comfortable and relaxed throughout surgery.
If you have particular worries, arrange to speak with the anesthesiologist before the day of surgery. These concerns don’t need to be logical or rational. Some people fear being put to sleep (as with general anesthesia) or worry that they might reveal personal secrets under anesthesia. Others fear having a needle in the back (as with regional anesthesia). Keep in mind that anesthesiologists spend a lot of time with unconscious people. Many of them welcome the opportunity to speak with an interested patient about his or her concerns.
 An IV will be started. Technically, it’s very simple—a prick or two of the skin is all it usually takes. But for individuals who are very frightened by needles, this may cause considerable worry. If you are anxious about the IV, let the nurse know, so that she or he can gently walk you through the experience.
An IV will be started. Technically, it’s very simple—a prick or two of the skin is all it usually takes. But for individuals who are very frightened by needles, this may cause considerable worry. If you are anxious about the IV, let the nurse know, so that she or he can gently walk you through the experience.
The IV is necessary for the intake of all fluids, including any medications and antibiotics, as well as sedation. The purpose of the sedative is to relax you and help make the procedure as comfortable as possible.
From this preparation area, you will be wheeled on a gurney or a wheelchair directly into the operating room. Your family or friends will not be allowed into the operating room, but will wait for you in a waiting room until after the procedure.
As you are brought into the operating room, you may notice how cool the temperature is. It is kept cool for two reasons. First, it is generally believed that the coolness helps minimize the possibility of infection. It is thought that bacteria don’t grow as well in a cool environment. Second, the surgeon must work under hot lights wearing a mask, a hat, gloves, and a gown. His or her need to stay alert is given priority. If you’re feeling cold, don’t hesitate to request a blanket.
Your anesthesiologist or nurse anesthetist will be with you throughout the surgery. In addition to administering the anesthetic, the anesthesiologist is essentially the general practitioner of the surgery experience. He or she not only provides pain control and monitor vital functions during surgery, but also is responsible for supervising your care immediately after surgery and discharging you from the recovery room. If you have questions or specific needs during the procedure, feel free to ask the anesthesiologist.
Your experience of the surgery, and what you remember about it depends, in part, upon the anesthesia. If you are having general anesthesia, you will be unconscious and unaware of the surgery. With an epidural or spinal, depending on your level of consciousness, you may be aware of a lot of activity and bright lights. You won’t be able to see the work directly, as a partition is put up. But you may be able to watch on a monitor. In general, you are likely to feel detached from the actual events. In addition, the anesthesia usually includes an amnesiac, so that you will have little direct memory or recall of the specific events.
Your doctor may perform the operation using arthroscopy, open surgery, or a combination of both. With arthroscopy, your surgeon makes a few small incisions in your knee—one for a fluid tube, one for a tiny scissors, scalpel, or drill, and another for an arthroscope (a very small instrument, about the size of a pen, containing a solid lens scope). A tiny camera transmits the image of your knee to a television monitor that is watched as the surgery is performed.
Your surgeon will obtain tissue from your own leg (unless he or she is using an allograft, which is tissue from a donor) as the material for the graft. A common procedure is to remove the central one third of the patellar tendon for the graft. It’s also common to use tissue from your hamstring for the graft. The specific type of graft that is used will depend on your medical circumstances. After small holes are drilled through the bone, the graft is threaded through these holes and the graft is then secured in place.
The time needed to complete the procedure varies widely from surgeon to surgeon. Generally, it takes between 45 minutes and three hours to complete.
Preparing for Departure
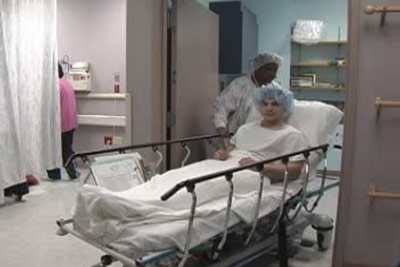
After surgery, you will be moved to a recovery room. Once your blood pressure, heart rate, and breathing are normal, you have urinated, and personnel in the recovery room think that you are ready to go, preparation will begin for your departure. If you are staying overnight, they will prepare to move you to your room.
There are times when a patient may be scheduled to leave the same day, but upon observation, the surgeon or other member of the medical team thinks that it is best to stay the night. This does not mean that something is wrong (15 years ago, patients routinely stayed for 3 or 4 days after ACL procedures) or that there are implications about the outcome of your surgery. It does mean, however, that your doctor believes that it is in your best interest to stay.
If you haven’t already received instructions, you will be informed about (a) the use of your brace, (b) the use of crutches to make sure you understand how to keep weight off your ACL leg as prescribed by your surgeon, (c) the icing protocol, and (d) the exercises you will need to do while at home until your formal physical therapy begins. You will also receive prescriptions for pain medication and general instructions to follow at home. It is important to have someone with you when you are getting prepared to go home, as you may find it difficult to remember some of these instructions due to lingering effects of the anesthesia.
