Reactions to Surgery
This section of the CD-ROM has basic information about how people respond to ACL surgery. Topics include normal physical reactions, complications, pain, and icing.
Normal Physical Reactions to Surgery
Like many other operative procedures, ACL surgery challenges the body in a number of ways. The following physical reactions to surgery are considered normal. There is no reason for alarm. If you believe that something is wrong, however, call your doctor’s office immediately.
You might run a low-grade fever (approximately 100.5ºF) for up to a week after surgery. A small amount of leaking (blood or other fluid) might seep from the wound. Your leg might be black and blue and show significant signs of bruising or discoloration. You might experience a degree of pain after surgery.
Complications
Call your physician if you experience any of the following complications:
•A rise in temperature above 101°F.
•Significant bleeding. It’s common for the dressing to have some staining, but if it is saturated, you need to call.
•Significant pain, especially if the pain grows progressively worse.
•Bothersome side-effects from the pain medication.
•Painful or red calf.
•Excessive dizziness.
•Continuous headache.
•Shortness of breath.
•A temperature that lasts for more than 72 hours.
What About the Pain?
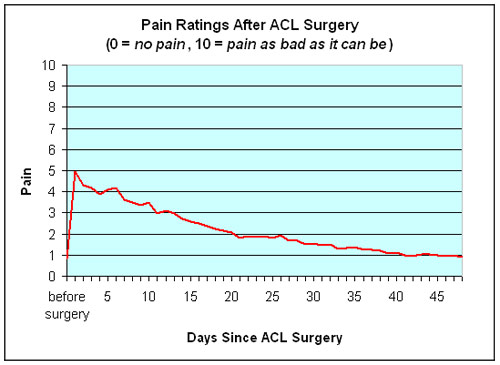 It’s normal to be worried about the pain of surgery. You know the pain that was involved in tearing the ligament; it’s typical to wonder what the reconstruction pain will be like. Fortunately, the repair—unlike the accident—will be done in a controlled setting. In the operating room, everything is done to minimize pain. In fact, regardless of the anesthesia used, you should not feel any pain during the procedure. In the days that follow surgery, whatever pain you might experience should be quite manageable. Research indicates that approximately 90% of patients describe their pain after ACL surgery as mild or moderate. As you can see from the graph, postoperative pain peaks the day after surgery and rapidly declines over the first few weeks after surgery to a level comparable to that experienced before surgery. Roughly 95% of patients report that their pain medication gave them good or excellent relief of pain after ACL surgery.
It’s normal to be worried about the pain of surgery. You know the pain that was involved in tearing the ligament; it’s typical to wonder what the reconstruction pain will be like. Fortunately, the repair—unlike the accident—will be done in a controlled setting. In the operating room, everything is done to minimize pain. In fact, regardless of the anesthesia used, you should not feel any pain during the procedure. In the days that follow surgery, whatever pain you might experience should be quite manageable. Research indicates that approximately 90% of patients describe their pain after ACL surgery as mild or moderate. As you can see from the graph, postoperative pain peaks the day after surgery and rapidly declines over the first few weeks after surgery to a level comparable to that experienced before surgery. Roughly 95% of patients report that their pain medication gave them good or excellent relief of pain after ACL surgery.
It’s important to note that everyone has their own individual threshold for pain, and some people do experience more relief from medication than others. In addition, many of us don’t call our doctor’s office even when we are in considerable pain. There are all kinds of reasons why this is the case. We may doubt what we are feeling: Am I just imagining or exaggerating the pain? We may worry that we will become addicted or fear that the doctor will think that we are trying to “score” some drugs. Or we may be afraid that the doctor will consider us wimps or hypochondriacs.
Although some pain is inevitable with surgery, there is no reason to tolerate ongoing pain that makes you miserable. Significant pain that is not properly controlled is more than just unpleasant—it can interfere with the healing process. Pain actually has an adverse effect on the functioning of the endocrine and immune systems. This means that the person who is in intense and constant pain after surgery is more likely to develop complications, have infections, or slow down the healing process. As a partner in the healing process, it is not just your right, but your responsibility, to let the doctor know that you are experiencing considerable pain after taking medication. Relief is available.
For some people, the assortment of discomforts associated with ACL surgery presents more of a challenge than the physical pain. For example, shortly after surgery, icing can seem never-ending…going to bed with a brace on can be uncomfortable and make sleeping difficult…the fear that someone or something will bang your leg can create a constant tension. People who have been through ACL reconstruction can offer some perspective. With the surgery behind them, it’s common for them to report that, in retrospect, this period of discomfort was actually quite brief and well worth the effort.
Icing
 In the days and weeks following surgery, icing (more technically referred to as cryotherapy or cold therapy) will become a regular part of your life. Icing lessens swelling and inflammation and helps to control pain. (Do not use heat on your knee; it tends to do the opposite—increase swelling, inflammation, and pain.) Your surgeon or other members of the medical staff will provide guidance about icing.
In the days and weeks following surgery, icing (more technically referred to as cryotherapy or cold therapy) will become a regular part of your life. Icing lessens swelling and inflammation and helps to control pain. (Do not use heat on your knee; it tends to do the opposite—increase swelling, inflammation, and pain.) Your surgeon or other members of the medical staff will provide guidance about icing.
Icing equipment for home use has become quite sophisticated: There are “systems” with thermostats that continuously pump cool water through a sleeve. (Some insurance companies will pay for these devices.) These circulating systems have their own ice chests, and are a way to keep the knee area continuously cold. For patients who don’t have access to one of these systems, there are freezable gel packs, homemade cold packs
(3 parts water, 1 part rubbing alcohol in gallon freezer bags), and, simpler still, ice in a plastic bag.
Icing recommendations will vary depending on the icing method used and the surgeon’s preference. Because your surgeon is most familiar with your particular needs, it is important to follow his or her guidelines.
Your formal program of icing may end when swelling, inflammation,
and pain are no longer concerns. However, icing is a valuable tool that can be used when you have stressed the knee in a way that results in swelling, inflammation, or pain. For example, many months after the conclusion of your rehabilitation program, icing is still a good idea
after a hard workout and/or physical therapy session, even if you do not expect any swelling. Icing is a good preventive technique that allows you to get the most from your workout as you achieve your recovery goals.
